Is There a Correlation Between Diabetic Retinopathy and Cataracts?
Do you have diabetes? Have you recently found out that you have cataracts as well?
You may not realize that by having diabetes, your risk of developing cataracts also increases. Patients with diabetes who have diabetic retinopathy are five times more likely to find out they have sight-threatening cataracts.
If you have type one or type two diabetes, managing your condition is key to having healthy eyes and good vision.
What is Diabetic Retinopathy?
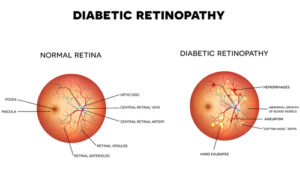
Diabetic retinopathy is a condition that occurs when your blood sugar levels stay too high due to diabetes. It arises when blood vessels in your retina are damaged because of high blood sugar levels.
Your eyes contain essential blood vessels that supply blood to the retina. When these blood vessels suffer damage, they can grow randomly, get blocked, or leak.
Damage to the blood vessels interferes with the blood supply to the retina, which makes it more difficult to see well. Diabetic retinopathy can seriously affect your eyesight in the later stages.
However, it often takes several years for the condition to get to where it threatens your sight. If it’s left undiagnosed and untreated, diabetic retinopathy can cause irreversible blindness. Other symptoms of the eye condition include experiencing:
- Poor night vision
- Blurred vision
- Blank areas in your field of vision
- Floaters
- Seeing colors as more faded than they are
If you have diabetes, you can lower your risk of developing diabetic retinopathy by:
- Attending all scheduled diabetic eye screening appointments. The sooner diabetic retinopathy is diagnosed, the better you’ll respond to treatment.
- Keeping your blood sugar levels, cholesterol, and blood pressure under control
- Contacting your eye doctor as soon as possible if you notice any vision changes
Cataracts
Cataracts develop when the natural lens of the eye becomes cloudy. The clouded lens causes blurred vision, increased sensitivity to light, halos, glares, and other frustrating visual symptoms.

While everyone will eventually get cataracts, people with diabetes are more susceptible to them. This is due to excess blood sugar that leads to a build-up of deposits on the eye’s natural lens.
If you have diabetes, your likelihood of developing cataracts increases two to five times. You also increase your chances of developing cataracts at an earlier age.
Cataracts progress more rapidly in people with diabetes than those who don’t have the condition. The reason is, high blood sugar that affects people with diabetes causes changes in your eyes, such as clouding of the lens or swelling, making it harder to see clearly.
Even though there’s no way to guarantee you’ll never have cataracts, you can lower your risk of getting the condition by keeping your blood sugar levels in check. Other preventative steps are:
- Going for dilated eye exams as recommended by your eye doctor
- Managing your cholesterol and blood pressure
- Quitting smoking if you’re a smoker
- Wearing polarized sunglasses to protect your eyes from harmful UV rays
Treatment for Diabetic Eye Disease
Diabetic eye disease comprises different eye conditions that can affect a person with diabetes. These conditions include diabetic retinopathy and cataracts.
When treating diabetic eye disease, your ophthalmologist will work with you to create a highly individualized treatment plan for the most optimal outcomes. Eye doctors and physicians recommend these steps to control your diabetes:
Take Medications as Prescribed
In some instances, your cholesterol or blood pressure medications can affect your blood sugar. It’s vital to take these medications exactly as prescribed or consult your doctor to change the dosages if your blood sugar increases too much.
Monitor Your Blood Sugar Levels

Discuss how often you should watch and record your sugar levels with your provider. Frequently testing your A1C levels can enable you to stay on track.
The test measures the blood sugar level attached to a protein that oxygenates the blood.
Live a Healthy Lifestyle

Include physical activity, such as walking, in your everyday routine. Additionally, eat fewer carbohydrates and add more fiber to your diets, such as nuts, whole grains, and antioxidant-rich vegetables and fruits.
Eye Medication
Some of the medications your ophthalmologist may administer during your visit are:
Corticosteroids to reduce inflammation caused by diabetic retinopathy
Anti-VEGF (Anti-Vascular Endothelial Growth Factor) therapy stops blood vessel growth in your retina and brings down retinal swelling
Eye Surgery
Sometimes, minimally invasive surgery is necessary to slow the progression of diabetic eye disease. The standard procedures used to treat diabetic eye disease are:
Vitrectomy
A vitrectomy is a surgical procedure to remove the blood and vitreous fluid that might leak from blood vessels. Your surgeon replaces the vitreous fluid with a saline substance to treat floaters.
Laser Surgery
During laser surgery, a surgeon will seal off or shrink blood vessels to minimize swelling in the retina.
Cataract Surgery
When cataracts get in the way of performing everyday tasks, your eye doctor may recommend having cataract surgery. Surgery is the only effective cataract treatment.
During the procedure, your cataract surgeon will remove the natural lens and replace it with an artificial one, called an intraocular lens (IOL). Many kinds of IOLs are available, depending on your goals and visual needs after cataract surgery.
If you choose a premium lens, you can reduce your dependence on glasses and contacts after cataract surgery. Many patients end up with their clearest and best vision after having cataract surgery with a premium lens.
Diabetic Eye Disease Specialists
Uncontrolled diabetes can cause vision loss and damage to your eyes. Dr. Tokuhara from Desert Vision Center works with diabetic patients to preserve and protect their vision.
Make sure diabetic retinopathy and cataracts don’t put your vision at risk by scheduling an appointment at Desert Vision Center in Rancho Mirage, CA.

