Glaucoma
Receiving a diagnosis that you are at risk for or have already developed glaucoma can be alarming, but it doesn’t have to be. At Desert Vision Center, we are experts at helping our patients manage their glaucoma and preserve vision.
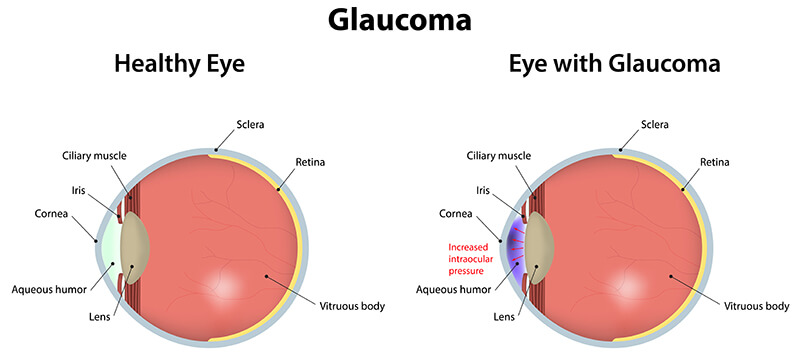
What is Glaucoma?
Glaucoma is a chronic and progressive eye disease that affects the optic nerve. It is often associated with older patients and affects approximately 3 million people in the United States. If the pressure inside the eye is too high or the optic nerve is sensitive, then untreated eye pressure in glaucoma can eventually lead to vision loss. Once this vision is lost, it cannot come back.
Who is Most Likely To Develop Glaucoma?
Some people may be more likely to develop glaucoma than others, like those with a family history of glaucoma. If you have a family history of glaucoma, it is important to let your eye doctor know.
Other Risk Factors:
- Elevated eye pressure
- Being nearsighted or farsighted
- Having health problems like diabetes, heart disease, and poor circulation
- Previous eye injury or trauma
If you are a higher risk of developing glaucoma, it is important to see your eye doctor more regularly. With routine eye examinations, your eye doctor can detect any early signs of glaucoma.
Symptoms of Glaucoma

There is a reason why glaucoma is sometimes called the silent thief of sight. In the earlier stages of the disease, there are often no visual symptoms. Elevated eye pressure does not always cause you to feel pain. As the disease progresses, there is a gradual, painless loss of vision.
Diagnosing Glaucoma
Early detection is critical in the diagnosis of glaucoma because many patients do not have any visual symptoms in the early stages of the disease. Left untreated, glaucoma causes damage to the optic nerve with irreversible vision loss.
There are several tests and clinical metrics used in the diagnosis of glaucoma. The most common is tonometry or the measure of the pressure inside your eye. The higher the pressure, the higher the risk of glaucoma damage may be.
Visual field testing involves computer mapping of your peripheral vision. Any functional damage from glaucoma can be detected by computerized or automated visual field tests. Optical coherence testing involves measuring structural damage to the optic nerve. When combined with visual field testing, both functional and structural changes are monitored through time to allow for the detection of glaucoma disease progression.
Treatment Options for Glaucoma
If you have glaucoma, there are several treatment options available to slow and prevent the progression of the disease. Because there are different forms of glaucoma and no two patients are identical, treatment options will vary person to person.
Prescription eye drops
Although there is no cure for glaucoma, prescription eye drops can lower the pressure in the eye to help prevent progression of glaucoma damage. Eye drops are not right for every patient. Some eye drops have side effects like blurred vision, redness, itching, or dry eyes.
Medicated Implant
Using eye drops for some patients can be problematic due to medication intolerance, difficulties with application of the eye drops (e.g. due to arthritis), high monthly co-payments, or trouble remembering to use the medication daily.
Durysta (bimatoprost) is a medicated dissolvable eye implant that slowly releases the therapeutic dose of glaucoma medication into the eye over the course of months. The procedure is quick and painlessly performed in the office.
Laser Eye Surgery
Another common way to treat glaucoma is with laser eye surgery. Laser surgery is an outpatient procedure. Different types of laser treatment options are available depending on the specific type of glaucoma that you have.
For open-angle glaucoma, laser trabeculoplasty is performed. The laser treats the trabecular meshwork or the part of the eye where pressure drains. For anatomic narrow-angle or closed angle glaucoma, laser iridotomy is used to help prevent eye pressure spikes. Finally, other specific glaucoma cases can be treated with cyclophotocoagulation laser. This laser treats the ciliary body or the part of the eye where the pressure is created.
Minimally Invasive Glaucoma Surgery (MIGS)
Minimally invasive glaucoma surgery is a broad category of surgical options used to help lower pressure in patients with glaucoma. These procedures utilize microscopic equipment and tiny incisions to lower eye pressure and prevent the progression of glaucoma with minimal complications. Typically, MIGS is done at the same time as cataract surgery, but can also be done as a stand alone procedure. Depending on your eye condition, Dr. Tokuhara may recommend MIGS surgery, such as iStent inject, OMNI Canaloplasty, Hydrus Microstent, or Kahook Dual Blade Goniotomy (KDB).

The iStent inject is a clinically proven microscopic glaucoma shunt. It is safely implanted in the eye during cataract surgery to allow aqueous eye pressure a clear path into the natural drainage area called Schlemm’s Canal. The iStent inject procedure is minimally invasive, with two separate titanium shunts. By using two shunts instead of one, multiple arcs of flow and collector channels are accessed allowing for improved results. Combination cataract with iStent inject surgery has an excellent safety profile comparable to cataract surgery alone. After surgery, many patients are able to stop or reduce the number of eye drops they use to treat their glaucoma.
The Hydrus Microstent is a minimally invasive stent about the size of an eyelash that is implanted into the eye during cataract surgery. In studies, 77% of Hydrus Microstent patients saw a significant reduction in eye pressure. It is placed into Schlemm’s Canal to provide scaffold and a direct flow of aqueous pressure into the collector channels. There are three windows in the stent that create a 90 degree scaffold to keep the canal open for clear and continuous outflow of pressure.
OMNI Canaloplasty (ab interno microcatheterization and transluminal viscodilation) is an implant-free MIGS procedure. A microcatheter is deployed through Schlemm’s Canal to open and break adhesions circumferentially 180 to 360 degrees. During retraction of the catheter, an internal reservoir in the device deploys viscoelastic into the canal to open the conventional outflow pathway.

The Kahook Dual Blade (KDB) is a device used to open the natural fluid drainage channel in the eye to lower eye pressure. The KDB opens the trabecular meshwork and allows open access to Schlemm’s canal for improved outflow of eye pressure. Unlike the iStent, there is no implant. Also, the KDB Goniotomy is covered by most insurances as a stand-alone procedure. In 2018, Dr. Tokuhara was the first surgeon in Coachella Valley to successfully perform the Kahook Dual Blade Goniotomy.
Glaucoma Surgery

For more advanced cases of glaucoma or when strict control of eye pressure is necessary, glaucoma surgery may be necessary. In these cases, a tube shunt is implanted to direct the pressure from inside the eye to an external reservoir implanted around the side of the eye. A commonly used tube shunt implant device is the Ahmed Valve, which looks like a miniature computer mouse with a flexible tube attached to the end of it. If you have advanced glaucoma and need surgery, call to schedule a consultation. Dr. Tokuhara has been performing Ahmed Tube implant surgery for over 10 years and has the experience you can trust.
Do I Need Glaucoma Surgery?
Not every patient who has glaucoma will need surgery. Many patients are able to keep their eye pressure controlled with either eye drops or laser. Surgery is necessary if eye drops are not enough to help control your eye pressure.
At Desert Vision Center, we are committed to preserving vision for patients affected by glaucoma. If you are at risk or have already been diagnosed with glaucoma and are interested in discussing treatment options, call our office to schedule a consultation.

